Phytoestrogens for Polycystic Ovary Syndrome (PCOS): Natural Approaches to Hormonal Balance
Published in IJPHDT, Vol-3, Issue-04, April-2026 (Vol. 3, Issue 4, 2026)
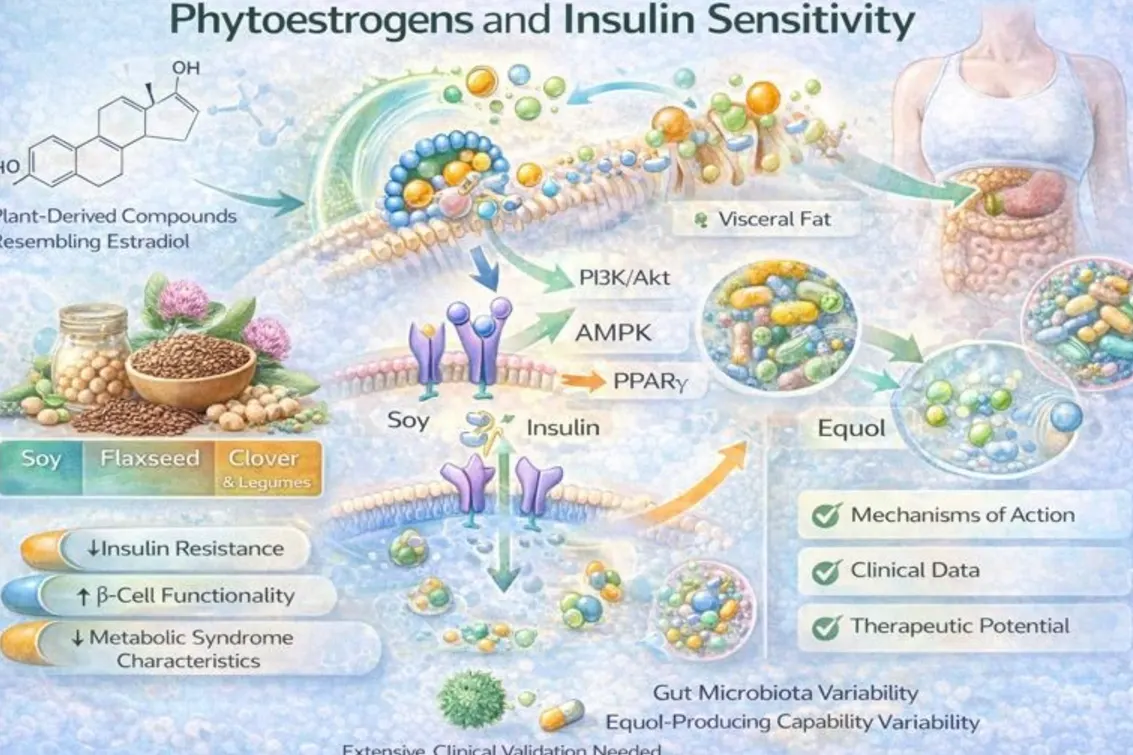
Abstract
References
- [1]1. Petrine, J. C. P.; Del Bianco-Borges, B. The Influence of Phytoestrogens on Different Physiological and Pathological Processes: An Overview. Phytotherapy Research 2021, 35 (1), 180–197. https://doi.org/10.1002/PTR.6816.
- [2]2. Villa, P.; Costantini, B.; Suriano, R.; Perri, C.; Macrì, F.; Ricciardi, L.; Panunzi, S.; Lanzone, A. The Differential Effect of the Phytoestrogen Genistein on Cardiovascular Risk Factors in Postmenopausal Women: Relationship with the Metabolic Status. J Clin Endocrinol Metab 2009, 94 (2), 552–558. https://doi.org/10.1210/JC.2008-0735.
- [3]3. Cederroth, C. R.; Vinciguerra, M.; Gjinovci, A.; Kühne, F.; Klein, M.; Cederroth, M.; Caille, D.; Suter, M.; Neumann, D.; James, R. W.; Doerge, D. R.; Wallimann, T.; Meda, P.; Foti, M.; Rohner-Jeanrenaud, F.; Vassalli, J. D.; Nef, S. Dietary Phytoestrogens Activate AMP-Activated Protein Kinase With Improvement in Lipid and Glucose Metabolism. Diabetes 2008, 57 (5), 1176–1185. https://doi.org/10.2337/DB07-0630.
- [4]4. HERBS AND SPICES - NEW PERSPECTIVES IN HUMAN HEALTH AND FOOD INDUSTRY. 2024.
- [5]5. Lee, C. C.; Bloem, C. J.; Kasa-Vubu, J. Z.; Liang, L. J. Effect of Oral Phytoestrogen on Androgenicity and Insulin Sensitivity in Postmenopausal Women. Diabetes Obes Metab 2012, 14 (4), 315–319. https://doi.org/10.1111/J.1463-1326.2011.01532.X;WGROUP:STRING:PUBLICATION.
- [6]6. Jungbauer, A.; Medjakovic, S. Phytoestrogens and the Metabolic Syndrome. J Steroid Biochem Mol Biol 2014, 139, 277–289. https://doi.org/10.1016/J.JSBMB.2012.12.009.
- [7]7. Kwon, D. Y.; Daily, J. W.; Kim, H. J.; Park, S. Antidiabetic Effects of Fermented Soybean Products on Type 2 Diabetes. Nutrition Research 2010, 30 (1), 1–13. https://doi.org/10.1016/J.NUTRES.2009.11.004.
- [8]8. Van Der Schouw, Y. T.; Pijpe, A.; Lebrun, C. E. I.; Bots, M. L.; Peeters, P. H. M.; Van Staveren, W. A.; Lamberts, S. W. J.; Grobbee, D. E. Higher Usual Dietary Intake of Phytoestrogens Is Associated with Lower Aortic Stiffness in Postmenopausal Women. Arterioscler Thromb Vasc Biol 2002, 22 (8), 1316–1322. https://doi.org/10.1161/01.atv.0000027176.83618.1a.
- [9]9. Talaei, M.; Pan, A. Role of Phytoestrogens in Prevention and Management of Type 2 Diabetes. World J Diabetes 2015, 6 (2), 271. https://doi.org/10.4239/WJD.V6.I2.271.
- [10]10. Ingram, D.; Sanders, K.; Kolybaba, M.; Lopez, D. Case-Control Study of Phyto-Oestrogens and Breast Cancer. Lancet 1997, 350 (9083), 990–994. https://doi.org/10.1016/s0140-6736(97)01339-1.
- [11]11. Rossouw, J. E.; Anderson, G. L.; Prentice, R. L.; LaCroix, A. Z.; Kooperberg, C.; Stefanick, M. L.; Jackson, R. D.; Beresford, S. A. A.; Howard, B. V.; Johnson, K. C.; Kotchen, J. M.; Ockene, J. Risk and Benefits of Estrogen plus Progestin in Healthy Postmenopausal Women. JAMA 2002, 288 (3), 321–333. https://doi.org/10.1001/jama.288.3.321.
- [12]12. Sites, C. K.; Toth, M. J.; Cushman, M.; L’Hommedieu, G. D.; Tchernof, A.; Tracy, R. P.; Poehlman, E. T. Menopause-Related Differences in Inflammation Markers and Their Relationship to Body Fat Distribution and Insulin-Stimulated Glucose Disposal. Fertil Steril 2002, 77 (1), 128–135. https://doi.org/10.1016/s0015-0282(01)02934-x.
- [13]13. Carr, M. C. The Emergence of the Metabolic Syndrome with Menopause. J Clin Endocrinol Metab 2003, 88 (6), 2404–2411. https://doi.org/10.1210/jc.2003-030242.
- [14]14. Pfeilschifter, J.; Köditz, R.; Pfohl, M.; Schatz, H. Changes in Proinflammatory Cytokine Activity after Menopause. Endocr Rev 2002, 23 (1), 90–119. https://doi.org/10.1210/edrv.23.1.0456.
- [15]15. DeFronzo, R. A.; Ferrannini, E. Insulin Resistance. A Multifaceted Syndrome Responsible for NIDDM, Obesity, Hypertension, Dyslipidemia, and Atherosclerotic Cardiovascular Disease. Diabetes Care 1991, 14 (3), 173–194. https://doi.org/10.2337/diacare.14.3.173.
- [16]16. Prasannarong, M.; Saengsirisuwan, V.; Piyachaturawat, P.; Suksamrarn, A. Improvements of Insulin Resistance in Ovariectomized Rats by a Novel Phytoestrogen from Curcuma Comosa Roxb. BMC Complementary and Alternative Medicine 2012 12:1 2012, 12 (1), 1–11. https://doi.org/10.1186/1472-6882-12-28.
- [17]17. Zamora-Ros, R.; Knaze, V.; Luján-Barroso, L.; Kuhnle, G. G. C.; Mulligan, A. A.; Touillaud, M.; Slimani, N.; Romieu, I.; Powell, N.; Tumino, R.; Peeters, P. H. M.; De Magistris, M. S.; Ricceri, F.; Sonestedt, E.; Drake, I.; Hjartker, A.; Skie, G.; Mouw, T.; Wark, P. A.; Romaguera, D.; Bueno-De-Mesquita, H. B.; Ros, M.; Molina, E.; Sieri, S.; Quirós, J. R.; Huerta, J. M.; Tjønneland, A.; Halkjær, J.; Masala, G.; Teucher, B.; Kaas, R.; Travis, R. C.; Dilis, V.; Benetou, V.; Trichopoulou, A.; Amiano, P.; Ardanaz, E.; Boeing, H.; Förster, J.; Clavel-Chapelon, F.; Fagherazzi, G.; Perquier, F.; Johansson, G.; Johansson, I.; Cassidy, A.; Overvad, K.; González, C. A. Dietary Intakes and Food Sources of Phytoestrogens in the European Prospective Investigation into Cancer and Nutrition (EPIC) 24-Hour Dietary Recall Cohort. Eur J Clin Nutr 2012, 66 (8), 932–941. https://doi.org/10.1038/EJCN.2012.36.
- [18]18. Viggiani, M. T.; Polimeno, L.; Di Leo, A.; Barone, M. Phytoestrogens: Dietary Intake, Bioavailability, and Protective Mechanisms against Colorectal Neoproliferative Lesions. Nutrients 2019, 11 (8). https://doi.org/10.3390/NU11081709.
- [19]19. Bennetau-Pelissero, C. Risks and Benefits of Phytoestrogens: Where Are We Now. Curr Opin Clin Nutr Metab Care 2016, 19 (6), 477–483. https://doi.org/10.1097/MCO.0000000000000326.
- [20]20. Domínguez-López, I.; Yago-Aragón, M.; Salas-Huetos, A.; Tresserra-Rimbau, A.; Hurtado-Barroso, S. Effects of Dietary Phytoestrogens on Hormones throughout a Human Lifespan: A Review. Nutrients 2020, Vol. 12, Page 2456 2020, 12 (8), 2456. https://doi.org/10.3390/NU12082456.
- [21]21. Wang, S.; Hu, Y.; Liu, B.; Li, Y.; Wang, M.; Sun, Q. Lignan Intake and Type 2 Diabetes Incidence Among US Men and Women. JAMA Netw Open 2024, 7 (8), e2426367. https://doi.org/10.1001/JAMANETWORKOPEN.2024.26367.
- [22]22. Farkas, S.; Szabó, A.; Hegyi, A. E.; Török, B.; Fazekas, C. L.; Ernszt, D.; Kovács, T.; Zelena, D. Estradiol and Estrogen-like Alternative Therapies in Use: The Importance of the Selective and Non-Classical Actions. Biomedicines 2022, 10 (4). https://doi.org/10.3390/BIOMEDICINES10040861.
- [23]23. Baudin, J.; Hernandez-Baixauli, J.; Quesada-Vázquez, S.; Mulero, F.; Puiggròs, F.; Arola, L.; Caimari, A. Combined Supplementation with Hesperidin, Phytosterols and Curcumin Decreases Adiposity and Improves Metabolic Health in Ovariectomized Rats. Food Funct 2024, 15 (9), 4905–4924. https://doi.org/10.1039/D3FO05122F.
- [24]24. Romani, A. M. P. The Controversy on the Beneficial Effect of Phytoestrogens in Diabetic Treatment in Postmenopausal Women. Biochem Pharmacol 2021, 190, 114619. https://doi.org/10.1016/J.BCP.2021.114619.
- [25]25. Glisic, M.; Kastrati, N.; Gonzalez-Jaramillo, V.; Bramer, W. M.; Ahmadizar, F.; Chowdhury, R.; Danser, A. H. J.; Roks, A. J. M.; Voortman, T.; Franco, O. H.; Muka, T. Associations between Phytoestrogens, Glucose Homeostasis, and Risk of Diabetes in Women: A Systematic Review and Meta-Analysis. Advances in Nutrition 2018, 9 (6), 726–740. https://doi.org/10.1093/ADVANCES/NMY048.
- [26]26. Cos, P.; De Bruyne, T.; Apers, S.; Vanden Berghe, D.; Pieters, L.; Vlietinck, A. J. Phytoestrogens: Recent Developments. Planta Med 2003, 69 (7), 589–599. https://doi.org/10.1055/S-2003-41122/ID/3/BIB.
- [27]27. Bateman, H. L.; Patisaul, H. B. Disrupted Female Reproductive Physiology Following Neonatal Exposure to Phytoestrogens or Estrogen Specific Ligands Is Associated with Decreased GnRH Activation and Kisspeptin Fiber Density in the Hypothalamus. Neurotoxicology 2008, 29 (6), 988–997. https://doi.org/10.1016/J.NEURO.2008.06.008.
- [28]28. Dixon, R. A. Phytoestrogens. Annu Rev Plant Biol 2004, 55 (Volume 55, 2004), 225–261. https://doi.org/10.1146/ANNUREV.ARPLANT.55.031903.141729/CITE/REFWORKS.
- [29]29. Delclos, K. B.; Bucci, T. J.; Lomax, L. G.; Latendresse, J. R.; Warbritton, A.; Weis, C. C.; Newbold, R. R. Effects of Dietary Genistein Exposure during Development on Male and Female CD (Sprague-Dawley) Rats. Reproductive Toxicology 2001, 15 (6), 647–663. https://doi.org/10.1016/S0890-6238(01)00177-0.
- [30]30. Iguchi, T.; Fukazawa, Y.; Uesugi, Y.; Takasugi, N. Polyovular Follicles in Mouse Ovaries Exposed Neonatally to Diethylstilbestrol in Vivo and in Vitro. Biol Reprod 1990, 43 (3), 478–484. https://doi.org/10.1095/BIOLREPROD43.3.478.
- [31]31. Losa, S. M.; Todd, K. L.; Sullivan, A. W.; Cao, J.; Mickens, J. A.; Patisaul, H. B. Neonatal Exposure to Genistein Adversely Impacts the Ontogeny of Hypothalamic Kisspeptin Signaling Pathways and Ovarian Development in the Peripubertal Female Rat. Reproductive Toxicology 2011, 31 (3), 280–289. https://doi.org/10.1016/J.REPROTOX.2010.10.002.
- [32]32. Ososki, A. L.; Kennelly, E. J. Phytoestrogens: A Review of the Present State of Research. Phytotherapy Research 2003, 17 (8), 845–869. https://doi.org/10.1002/PTR.1364.
- [33]33. Brandenberger, A. W.; Tee, M. K.; Lee, J. Y.; Chao, V.; Jaffe, R. B. Tissue Distribution of Estrogen Receptors Alpha (ER-α) and Beta (ER-β) MRNA in the Midgestational Human Fetus. J Clin Endocrinol Metab 1997, 82 (10), 3509–3512. https://doi.org/10.1210/JCEM.82.10.4400.
- [34]34. Cimafranca, M. A.; Davila, J.; Ekman, G. C.; Andrews, R. N.; Neese, S. L.; Peretz, J.; Woodling, K. A.; Helferich, W. G.; Sarkar, J.; Flaws, J. A.; Schantz, S. L.; Doerge, D. R.; Cooke, P. S. Acute and Chronic Effects of Oral Genistein Administration in Neonatal Mice. Biol Reprod 2010, 83 (1), 114–121. https://doi.org/10.1095/BIOLREPROD.109.080549.
- [35]35. Jefferson, W. N.; Couse, J. F.; Padilla-Banks, E.; Korach, K. S.; Newbold, R. R. Neonatal Exposure to Genistein Induces Estrogen Receptor (ER)α Expression and Multioocyte Follicles in the Maturing Mouse Ovary: Evidence for ERβ-Mediated and Nonestrogenic Actions. Biol Reprod 2002, 67 (4), 1285–1296. https://doi.org/10.1095/BIOLREPROD67.4.1285.
Authors (5)
Jai Shankar Pandey
Faculty of Nursing and Paramed...Faculty of Nursing and Paramedical, Mahayogi Gorak...Faculty of Nursing and Paramedical, Mahayogi Gorakhnath University Gor...Faculty of Nursing and Paramedical, Mahayogi Gorakhnath University Gorakhpur, Gorakhpur, Uttar Prade...
View all publications →Prashant Kumar
Guru Shree Gorakshnath Chikits...Guru Shree Gorakshnath Chikitsalay Gorakhpur, Utta...Guru Shree Gorakshnath Chikitsalay Gorakhpur, Uttar Pradesh, IndiaGuru Shree Gorakshnath Chikitsalay Gorakhpur, Uttar Pradesh, India
View all publications →Aditya Kumar Jaiswal
Faculty of Nursing and Paramed...Faculty of Nursing and Paramedical, Mahayogi Gorak...Faculty of Nursing and Paramedical, Mahayogi Gorakhnath University Gor...Faculty of Nursing and Paramedical, Mahayogi Gorakhnath University Gorakhpur, Gorakhpur, Uttar Prade...
View all publications →Rohit Rajak
Faculty of Nursing and Paramed...Faculty of Nursing and Paramedical, Mahayogi Gorak...Faculty of Nursing and Paramedical, Mahayogi Gorakhnath University Gor...Faculty of Nursing and Paramedical, Mahayogi Gorakhnath University Gorakhpur, Gorakhpur, Uttar Prade...
View all publications →Shubham Kumar Maurya
Faculty of Nursing and Paramed...Faculty of Nursing and Paramedical, Mahayogi Gorak...Faculty of Nursing and Paramedical, Mahayogi Gorakhnath University Gor...Faculty of Nursing and Paramedical, Mahayogi Gorakhnath University Gorakhpur, Gorakhpur, Uttar Prade...
View all publications →Download Article
Best for printing and citation
Download Article
Best for printing and citation
Article Information
IJPHDT430013
IJPHDT-01-000243
127-173
2026-04-28
Article Impact
Smart Citations
scite shows how a scientific paper has been cited by providing the context of the citation, a classification describing whether it supports, mentions, or contrasts the cited claim, and a label indicating in which section the citation was made.
How to Cite
Shankar, J., & Kumar & Kumar, A. & Rajak & Kumar, S. (2026). Phytoestrogens for Polycystic Ovary Syndrome (PCOS): Natural Approaches to Hormonal Balance. International Journal of Pharmacognosy and Herbal Drug Technology, 3(4), 127-173. DOI:https://doi.org/10.64063/3049-1630.vol3.issue4.000243
Article Actions
More from this Issue
Foxnut as a Natural Laxative: Study on Its Efficacy and Mechanism in Constipation Management
Formulation and Evaluation of Herbal Vitamin C Serum from Orange Peel Extract
From Folklore to Pharmacy: Bridging Ethnobotany and Modern Drug Discovery through In Vitro Screening
More by These Authors
Standardization and Quality Control of Ayurvedic Polyherbal Formulations
2025 • Vol. 2, Issue 7
Read more →
